Transforming construction health and safety with SHINe
RMIT has launched the Safety and Health Innovation Network (SHINe), an industry-led collaborative research funding model to identify and tackle problems across the construction industry.
Gold beats platinum for chemo drugs in new lab study
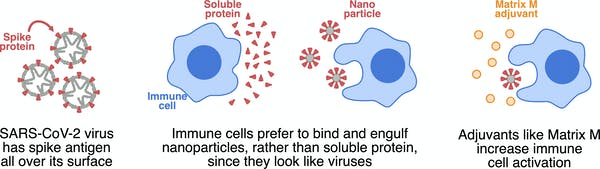
Gold-based drugs can slow tumour growth in animals by 82% and target cancers more selectively than standard chemotherapy drugs, according to new research out of RMIT University.
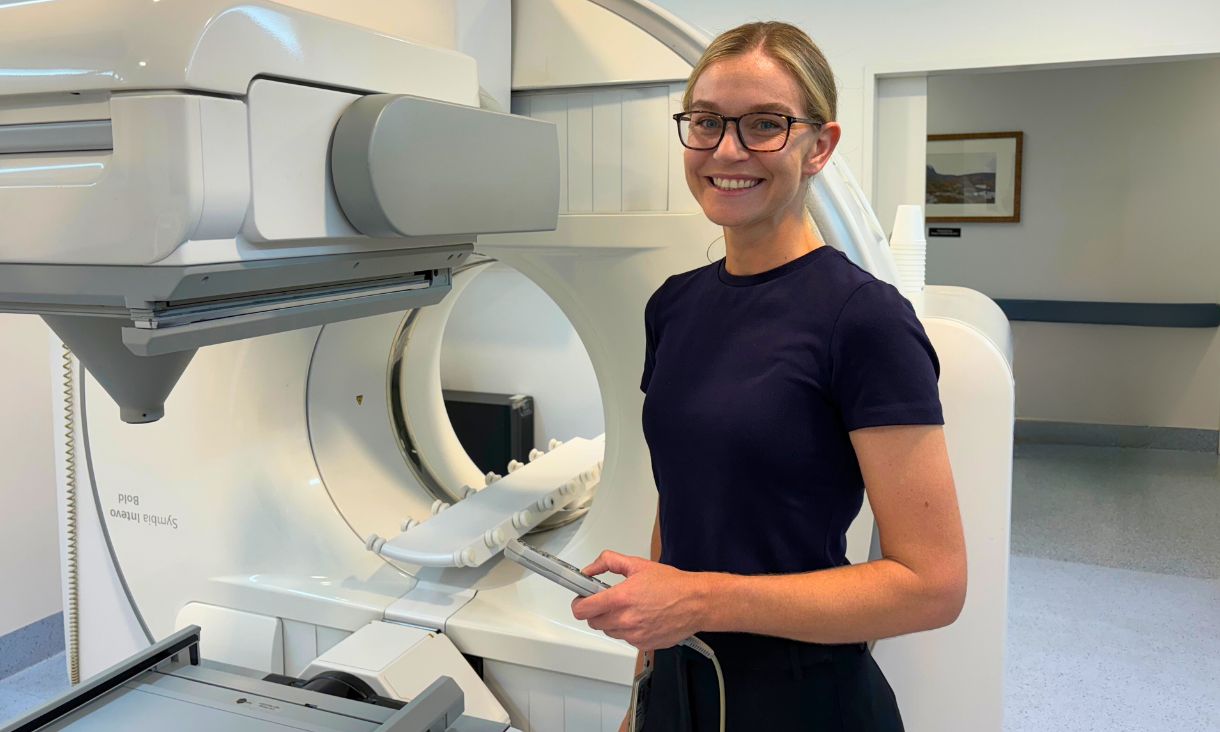
RMIT responds to critical skills shortage to support early cancer diagnosis in Queensland
RMIT University will offer Queensland’s first nuclear medicine degree, addressing critical workforce shortages and shoring up cancer services across the state.
New partnership with Cisco and Grampians Health to upskill healthcare sector
RMIT’s Health Transformation Lab and College of Vocational Education are piloting a program to rapidly upskill front-line staff, broader health workforce and IT professionals in the healthcare sector to meet the industry’s emerging skills needs.